Pregnancy is a life-altering experience, transforming your mind, body, and spirit from the inside out. The last thing you want to deal with when you are literally growing a human is someone spouting myths about being plus size and pregnant. I chatted with a few maternal care specialists about the most common plus size pregnancy myths and the real information plus size pregnant people need to know for a healthy, happy experience.
Why Debunk Plus Size Pregnancy Myths?
Researchers Erin Basinger and Margaret Quinlan took a look at fat shaming in maternity care and found that 77.2% of the memorable messages fat people received before, during, and after pregnancy were negative. There were three core negative messages found through their analysis:
- Body size is the primary reason for infertility
- Weight loss will lead to a successful pregnancy
- Refusal of care
Facing negative, incorrect, and oftentimes unsolicited commentary about your body and pregnancy is a surefire way to drive stress levels up and negatively impact your experience. Christine Dunkel Schetter and Lynlee Tanner’s research review shows medical professionals agree– stress, anxiety, and depression are not good for a pregnancy.
So, we found 5 of the most outrageous plus size pregnancy myths, and debunked them because you deserve to have a happy, stress-free experience.
5 Plus Size Pregnancy Myths Debunked

Myth #1: People with a high body mass index (BMI) can’t get pregnant
Let’s start with the fact that BMI is deeply flawed. It assumes fat people are automatically unhealthy, which is objectively incorrect. A better indication of whether you will have some sort of fertility complication is your medical history and pre-existing conditions rather than just weight. Many different things cause infertility, and 1 in 4 couples can’t identify the specific reason why.
Nicola Salmon, who goes by @fatpositivefertility on social media, shared in my frustration about this myth saying, “There has been no biological mechanism proven to explain this idea and there are so many fat folks that get pregnant really easily. If this were a fat person problem, why doesn’t it happen to all fat people?”
She continues, “What CAN happen is the stigma that fat people experience leads to both an increase in their stress levels and a decrease in access to care. An increase in stress levels can increase stress hormones, impacting reproductive hormones and increasing inflammation.
Combining the additional stress with decreased access to care means potential issues may not be diagnosed or treated until much later, if at all. There are so many BMI barriers placed on fertility care that it can become a stressor in itself to be able to access the care that you might need.”

Myth #2: You Cannot Have A “Typical Vaginal Birth” Over A Certain Weight
We asked Salmon to tell us the weirdest myth she has come across regarding plus size pregnancy, and she said, “The weirdest myth I’ve heard is that fat people can’t have unassisted births because they have fat vaginas and the babies can’t get out. I wish I was joking! Fat people have been having babies for millennia and will continue to have boring and ordinary pregnancies and births without intervention if that’s what they choose.”
The American College of Gynecology (ACOG) claims that overweight individuals have longer labors and it can be harder to monitor the fetus during labor. For these reasons, there is an increase in having a cesarean section (c-section) birth if you are plus size.
While studies do show longer labor at a higher weight, the increase is small; approximately 1.5hrs. This also brings up the question- how can we expect it to be easy to monitor plus size folks while pregnant when the monitors are not made for plus size bodies?
External fetal monitors typically don’t work as well on plus size bodies. Because of your belly shape, it may be harder to position. Wireless monitors like the Novii Wireless Path System tend to work better because they WERE designed with plus size bodies in mind. The issue is they aren’t available at all facilities.
Myth #3: You Are Automatically Considered High-Risk If You Are Plus Size
In spite of what some health care providers think, plus size pregnancy does not automatically mean you will experience complications. Often, increased pregnancy risks are associated with other conditions and diseases like gestational diabetes (GD), hypertension, and preeclampsia.
Salmon shared numbers with us to help put some of the information in context. “For example, approximately 2% of folks with a BMI of 19-25 get diagnosed with Gestational Diabetes. About 10% of folks in the highest BMI bracket are diagnosed. That means 90% of those in the highest BMI bracket DON’T get it.”

Nicola explains, “It’s important to be aware of the chance of complications occurring during pregnancy but an automatic label of “high-risk” is both inaccurate and harmful. Who decides what high-risk even means? The research around the increased incidence of complications based on BMI is not conclusive, but even if we take the worst case scenario data, the way that the majority of providers talk about risk is fear mongering. Take for example gestational diabetes- approximately 2% of folks with a BMI of 19-25 get diagnosed with GD, folks in the highest BMI bracket are at about 10%, which means that 90% of those in the highest BMI bracket DON’T get it.”
These complications are risks for patients of all sizes, including those of an ‘ideal’ weight. There are things you can do to reduce those risks without being required to lose weight. Just adding exercise, like taking walks, and reducing processed foods can help lower your risks.
Nicola continues, “It’s important to be aware of the chance of complications occurring during pregnancy, but an automatic label of “high-risk” is both inaccurate and harmful. Who decides what high-risk even means? The research around the increased incidence of complications based on BMI is not conclusive, but even if we take the worst case scenario data, the way that the majority of providers talk about risk is fear mongering.”
Myth #4: You Can Give Birth Anywhere
We recommend checking with your team at the facility you want to give birth at, whether it’s the hospital, birthing center, or even your midwifery support staff. Some providers and hospitals will tell you they have a BMI cut-off for labor and delivery.
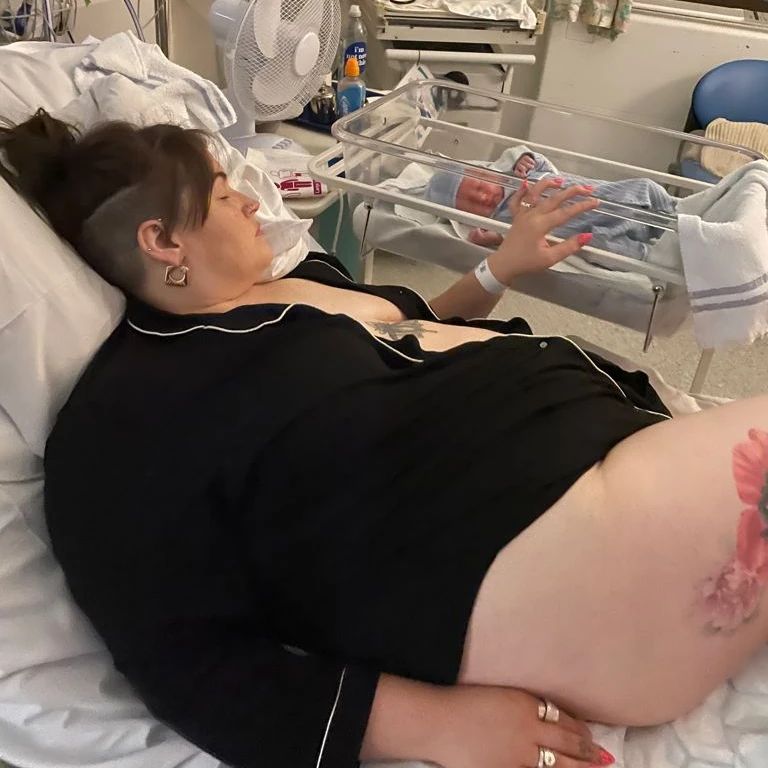
Myth #5: You Won’t Look Pregnant If You’re Already Fat
Plus size pregnancy can bring up a lot of issues surrounding body image. Some plus size folks end up having a perfectly rounded out “D” shaped belly, while others will not experience that and have a “B” shaped belly instead.
Because there is so little representation of what fat bodies look like while pregnant, it is possible that some people in your life may not notice your pregnant belly. This can be harmful when a co-worker makes a comment like “oh my gosh, you’re pregnant? I had no idea!” while you’re discussing your plans for a C-section because your baby is breech.
This also causes a lot of women to not fully embrace their plus size pregnant body, avoiding all photographs. Maternity photos have become such a growing trend over the last decade and many plus size women regret not taking photos of their pregnancy. So if there’s one recommendation we have for you during your pregnancy journey, it is to TAKE THE PICTURES!!!

Plus size pregnancy myths are just that– myths
A study by Erin Basinger, Margaret Quinlan, and Audrey Curry analyzed survey responses from fat individuals who have tried to conceive, have been pregnant, or had a child. “The two most prevalent pieces of advice were to trust yourself and your body and find an inclusive provider. Based on our results, we suggest finding fat-affirming and inclusive providers, seeking nourishment rather than a restrictive diet, engaging in joyful movement, and connecting with a community of other fat individuals.”
Find a provider and birthing facility that works for you, your baby, and your body. Salmon suggests crowdsourcing for recommendations in order to find fat positive medical providers for your pregnancy. Ask your fat friends! There are also a few fat-positive communities and resources like Size Friendly Directory (fat-friendly doulas) or Fat and Pregnant (a Facebook-based support group). If you aren’t able to find one using those resources, asking a few questions from a local OB/GYN’s office such as:
- Do you routinely recommend weight loss to patients?
- Do you have any specific BMI-related policies within your practice?
- How do you screen for eating disorders?
- Do you routinely weigh clients?
This is a good way to get an indication of how they treat their plus size patients.
We hope in the future, the American College of Obstetrics and Gynecologists (ACOG) will update their guidelines for plus size pregnancy based on more current research. The AMA’s recommendation that physicians not use BMI as a sole indicator of health is a step in the right direction, but there is still so far for us to go to receive equitable, evidence-based care.
A plus size body doesn’t automatically equal an unhealthy pregnancy and if your provider makes you feel unsupported or shamed, you have every right to find a new one. And if you’re already in the market, check out our recommendations about how to find a fat-friendly doctor.







